
As countries around the world invest in Biosafety Level 4 laboratories to study lethal viruses and prepare against unknown pathogens, some scientists are sounding the alarm about the potential for a catastrophic accident or attack.
Story by Eduardo Baptista, Linda Lew, Simone McCarthy and Peter Langan
Andreas Kurth has an unusual, and uncomfortable, dress code for his job.
Encapsulated in an inflatable bodysuit, his frizzy grey curls wrapped in a skullcap or bandana, Kurth breathes air at a humidity of about 5 per cent, far drier than in the Sahara Desert, to help prevent bacteria forming in the air hoses. A couple of hours in the suit leads to dehydration and discomfort, but it’s the rubber gloves that bother him most. He wears three pairs, but needs hand dexterity to unscrew the tops of small vials and then screw them back on again.
“They have to be tight enough that we can unscrew a vial of samples,” he says, “but they can’t be so tight to the point we can’t move our fingers.”
Being able to handle the vials is essential. They contain death.

The 47-year-old heads the Biosafety Level 4 laboratory at the Robert Koch Institute in Berlin, Germany, the type of lab that handles viruses capable of sickening or killing humans in their millions. It is the front line in the world of virology, where men and women in astronaut-like suits explore a microscopic space to deconstruct the genetic code of deadly viruses. The goal is to mount counter-attacks using tailor-built vaccines and antiviral drugs.
If “know your enemy” is the maxim to survive conflict, taking on a potentially fatal virus as an adversary, like those that cause Ebola, Aids or Covid-19, throws up especially difficult challenges. This invisible enemy is immune to reason, mutates as it spreads, and multiplies in hosts it infects before launching attacks on more people. And viruses exist in uncountable billions.
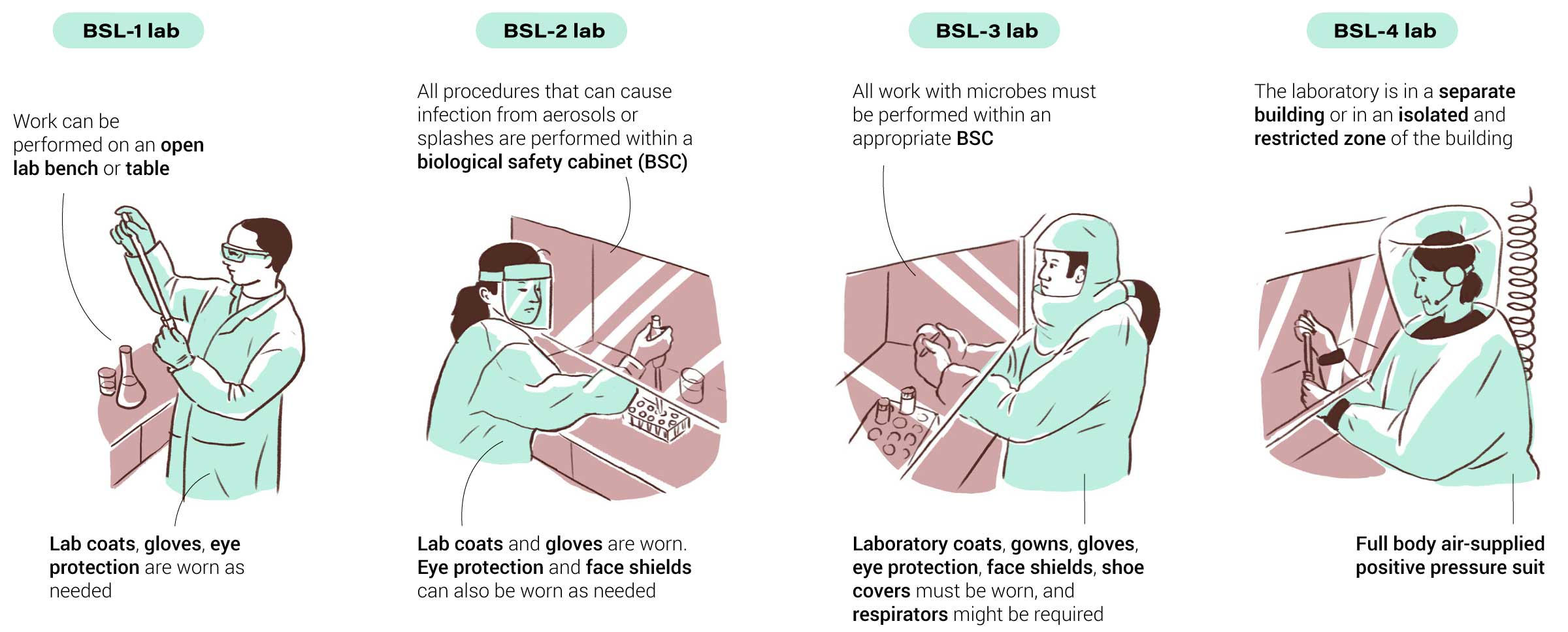
Labs handling micro-organisms are classified from Biosafety Level 1 to the Level 4 facilities, such as Kurth’s, that research the deadliest pathogens known to medical science. And they do not come cheap. Besides the expense of building BSL-4 labs, microscopes for virus research can cost more than US$500,000 each, says Kurth. He estimates that his Berlin lab required an outlay of as much as €20 million (HK$183 million) to build. Yearly expenses to keep the labs secure and running safely can be as much as 10 per cent of construction costs, according to some estimates.
BSL-4 researchers have also taken the fight beyond the lab, out into the midst of epidemics.
Containment requirements and safety equipment for laboratories of different levels
In 2014, Kurth spent four weeks in Guéckédou, Guinea, ground zero for the worst Ebola outbreak in human history during which, according to the World Health Organisation, more than 11,000 people died from the virus in West Africa. Each day Kurth would test blood samples for Ebola and he saw many people perish, children among them, but he would do it again. “I feel it as a mission,” he says, “or a duty basically, because I am trained to work with Ebola, so who else should go there if not me?”
At Kurth’s ground-level lab in an industrial district of Berlin, he and his staff of 15 work in an area of about 330 square metres, roughly two-thirds the size of a basketball court, communicating through headsets inside their suits. Walls, cables and pipes are built airtight in the four-storey structure and any airborne particles are sucked out by giant exhaust filters that replace the lab’s air 10 to 15 times an hour.
An entire floor above the lab is packed with air exhaust pipes, and the floor above that is occupied by an air-conditioning system that filters the air coming in and out. The floor below the lab houses a backup power supply and a unit for treating waste water. The building also has a furnace for burning solid waste – including defunct computers – the air from which is pumped through another incinerator before being filtered out.
“For Level 4 the requirement is that for every technical unit you have a redundant unit, so for everything you build and plan you have a second structure that takes over if the first one fails,” says Kurth.
Researchers moving in and out of an airlocked BSL-4 lab face other challenges. Before entering, they must strip from head to toe – not even contact lenses are allowed in – and slip on a full-body jumpsuit. Kurth jokes that the time it takes to enter and exit the lab depends on how many piercings and pieces of jewellery a researcher wears.
The wearer’s socks and gloves are taped to the jumpsuit before they wriggle into the protective cocoon. “We want to minimise the contact of the skin with the suit,” Kurth says. “The inflatable suit is in contact with the contaminated laboratory, we want space between this layer and our body.”
The lab is exited via two showers. The first is taken in a wardrobe-sized room at the airlocked entrance where the researcher is sprayed with Micro-Chem Plus, a detergent disinfectant used in BSL-4 labs around the world. There is nothing special about the cleaner. Most viruses are enveloped in a layer of fat that soap breaks down, killing the pathogen. The detergent works in much the same way as washing-up liquid removes grease from dishes. This is why medical authorities urge hand-washing with soap to prevent infection with the virus that causes Covid-19.
Once the shower timer hits six minutes, the door automatically unlocks and the researcher can strip off the lab suits, which are washed and reused. Then there is a second shower before the changing room can be entered.

Such working conditions can make recruitment difficult, says Kurth. But, he adds, “we don’t want anyone working in BSL-4 because they find it cool and risky; we want people that are very calm, both feet on the earth.”
Selecting the right people helps to prevent accidents and ensure that bad actors don’t get hold of deadly viruses. Both have already happened at BSL labs.
In 2004, a Russian scientist working on an Ebola vaccine in a BSL-4 lab in Siberia died after pricking her hand with a syringe used to draw blood from guinea pigs infected with the virus. Bruce Edwards Ivins, a researcher at the Fort Detrick military base, in Maryland, home to one of the world’s first biological high-containment labs, committed suicide in 2008. The FBI later said Ivins was a suspect in the 2001 mailings of letters containing anthrax to American senators and media outlets, killing five people and infecting 17.
Dr David Franz, former commander of the US Army Medical Research Institute of Infectious Diseases at Fort Detrick, said that BSL-4 labs require similar security to nuclear weapon facilities – “guns, gates and guards” – as well as biological safety in the lab. Franz, 74, spent 23 years in army biological research before retiring in 1998.
No laboratory can be 100 per cent safe, he says, echoing Kurth in Berlin in stressing the need to foster a culture of trust and accountability among staff.
Natural disasters are another risk for BSL-4 labs. The US Centres for Disease Control and Prevention is to build a US$400 million BSL-4 lab in Atlanta, and the US$1.2 billion National Bio and Agro-Defence Facility under construction in Kansas by the Department of Homeland Security will also include a BSL-4 lab, expected to be fully operational by late 2022.
“There have to be strict safety requirements about where these are located to avoid creating hazardous conditions near densely populated areas or areas that are prone to flooding, or typhoons, or earthquakes,” says Gregory Koblentz, a biodefence researcher at George Mason University, in Virginia.
During the construction of the Berlin facility, Kurth says engineers simulated an aircraft crashing into the laboratory and found the viruses would not survive the fire of the explosion. “Pathogens are in freezers that are kept under lock and key,” he says. “They’re not in some soda machine that if it falls down all the samples break.”
Science tells us humankind lives in a virtual soup of micro-organisms that propagate in water, food, soil and air, but not all are harmful. Untold numbers live in the human gut and are essential to digestion, absorbing nutrients from food. Others are present for reasons researchers still do not understand.
The word “virus” is usually associated with “disease”, or pathogens such as HIV, Ebola, Zika and influenza, according to the 2017 report “The Good That Viruses Do”, published in the Annual Review of Virology. “However, as we are now finding out, not all viruses are detrimental to human health,” write the authors Mario Mietzsch and Mavis Agbandje-McKenna, virologists at the University of Florida.
Good viruses are not what brought Kurth into virology. As a 21-year-old biology undergraduate, he backpacked through East Africa and became infected with parasitic lungworms. That saw him hospitalised for three months. The episode hooked Kurth on the study of parasites, and later viruses, and eventually of BSL-4 pathogens such as Ebola.
Public health officials and virologists have warned for decades about the growing risk from outbreaks of unknown and harmful viruses. Some point to the doubling of the global human population to 7.8 billion since the 1960s as one reason for that escalating threat.
“We are densely packed, we’re exploiting pristine environments, we are creating and driving the ecologic pressure that is creating the risks that are driving the risk at the animal/human species barrier,” said Mike Ryan, executive director of WHO’s Health Emergencies Programme, at a press briefing on August 10. “We live on a planet in which we’re adding a billion people a decade.”

The need to feed this population has revolutionised food production, driving the destruction of animal habitats to make way for crops and livestock, and increasing the threat. The WHO estimates 70 per cent of new human disease outbreaks in the past 50 years have been zoonotic, originating in animals.
The WHO’s annual disease preparedness plan in 2018 provided a list of deadly pathogens posing the greatest risk to public health. It included Ebola and severe acute respiratory syndrome, and at the bottom of the list, the WHO added Disease X, a warning about the outbreak of an as yet unknown virus with the potential to infect and kill humans. Covid-19, researchers have said, fits the description.
As health authorities advise on basic defences against the virus that causes Covid-19 – including washing hands, wearing masks, social distancing and quarantine – the hunt is on for a vaccine.
With billions of dollars being funnelled into companies such as Moderna and AstraZeneca to develop a vaccine for Covid-19, governments are also looking to BSL labs as a vanguard in the fight against possible future unknown viruses.
That means building more of them. But not all scientists agree with that strategy or the types of research sometimes conducted in high-containment labs. Globally, there are 54 BSL-4 labs, either in operation or under construction, spread throughout Asia, Africa, Europe, Russia and the US, according to a 2017 WHO report.
The US has the largest number of operational BSL-4 labs, with 10. It is also in the US that researchers over the past 70 years have set the procedures and safety standards for how to build and run labs to investigate deadly pathogens. That leading role can be traced in part to Nazi Germany, the Nuremberg trials and Japan’s Unit 731, which conducted biological warfare in China during World War II.
Germ warfare
After the war ended, in 1945, as many as 199 Nazi officials faced trials in Nuremberg, Germany, on charges including war crimes and crimes against humanity. Among the cases heard was the so-called Doctors’ Trial of 23 medical personnel. The charges included conducting forced biological and medical experiments on thousands of inmates at concentration camps, such as Ravensbrück and Auschwitz. These experiments included infecting prisoners with such diseases as tuberculosis, malaria and yellow fever during research into the use of biological agents as weapons of war.
Seven of the doctors were convicted and hanged on June 2, 1948, nine faced imprisonment, while seven were acquitted. The doctors were tried before a US military court in Nuremberg, which meant that the extensive records of the biological experiments fell into American hands.
Japan also conducted biological and chemical research during WWII, much of it in Harbin, according to documented accounts. It included forced medical experiments on prisoners as well as attacks against civilians in China using biological agents such as typhoid, smallpox and plague-infected fleas. The unit involved was officially called the Epidemic Prevention and Water Purification Department, but is better known as Unit 731. It was effectively a biological warfare operation led by soldier and microbiologist General Shiro Ishii, whose use of biological weapons in China is estimated to have killed or injured hundreds of thousands of people.
However, unlike the Nazi doctors, Ishii and others involved in Unit 731 escaped prosecution by the US at the Tokyo War Crimes Trials (1946-48), the equivalent in Japan to Nuremberg. According to now declassified documents, US military authorities granted members of Unit 731 immunity from prosecution in return for data they had gathered on biological warfare.
Securing troves of documents on the methods and means of developing biological weapons, their results when used in military attacks, and the individuals who developed them, took on a new significance as the US faced a new adversary in the Soviet Union, and biological warfare was seen as a real threat.
In her 2017 book, Hidden Atrocities: Japanese Germ Warfare and American Obstruction of Justice at the Tokyo Trial, medical anthropologist Jeanne Guillemin says the US military obtained biowarfare documents from Unit 731. And most, if not all, of the Nazi and Unit 731 data that made its way to America ended up at Fort Detrick, home to one of the world’s oldest BSL-4 labs, where the US military ran its biological warfare research programme for more than two decades before it was terminated, in 1969, by President Richard Nixon.
The procedures developed at Fort Detrick later served as the basis for the US Centres for Disease Control and Prevention’s publication Biosafety in Microbiological and Biomedical Laboratories, considered the biosafety bible in labs worldwide.
“Thus, in what we might today call a reverse dual use model, some very important good – lab safety – has ultimately come from a programme that was designed to do harm,” Franz says.

Something else came out of the trial of the Nazi doctors in Germany in 1947: the Nuremberg Code, a list of 10 ethical principles to guide medical research and treatment of patients, written to counter the exploitation, suffering and murder of prisoners in the name of science and ideology in Nazi concentration camps. It remains one of the most influential documents on clinical work.
These principles state that voluntary consent is essential, and the results of any experiment must be for the greater good of society. Principle number six is that the risks should never exceed the benefits. It is this question – do the risks exceed the benefits? – that has split the medical research community in relation to the type of work that takes place today in BSL-3 and BSL-4 labs.
Specifically, this involves the creation of new strains of viruses in the name of research, according to a 2014 statement opposing the work and signed by more than 300 scientists. Known as the Cambridge Working Group Consensus Statement, it called for a halt to what is known as gain-of-function research, which can involve taking an existing virus and giving it new attributes, potentially making the pathogen more dangerous.
“Laboratory creation of highly transmissible, novel strains of dangerous viruses, especially but not limited to influenza, poses substantially increased risks,” the Cambridge Working Group statement says. It points to “incidents” at US labs involving viruses such as anthrax and the “fallibility of even the most secure laboratories”.
The argument about gain-of-function research blew up in 2012 after two labs, in the Netherlands and in Wisconsin, published research showing they had created H5N1 influenza virus strains that were transmissible between ferrets, which have respiratory systems similar to those of humans. Part of the rationale for the work was disagreement over whether H5N1, or bird flu, usually spread by chickens and wildfowl, could be transmitted by mammals.
A 2014 editorial in mBio, a journal published by the American Society for Microbiology, argued that the work carried out by the labs was essentially a “species jump” that gave a virus the capability to transmit between mammals, something it had previously lacked.
Gain-of-function research has also been conducted on coronaviruses, the family from which Covid-19 sprang. This work on coronaviruses disturbs Amir Attaran, a professor in the faculty of law and School of Epidemiology and Public Health at the University of Ottawa, in Canada. He is one of the original signatories and a founding member of the 2014 Cambridge Working Group.
If you take one of those lesser human coronaviruses and you combine its host range with a bat coronavirus from the wild having more aggressive properties, more virulent properties, you could end up with something that is very, very dangerous.Amir Attaran, lawyer and biologist
“You are in an area of research [that] were a mistake to be made, you could be introducing into the world and to billions of people, something at least as bad, if not worse than the virus causing Covid-19.”
Supporters of gain-of-function research argue it is necessary to improve detection of dangerous viruses and facilitate vaccine development against future pandemics. Attaran argues the emergence of Covid-19 undermines this view.
“We’ve done gain-of-function research on coronavirus,” he says. “It didn’t prepare our surveillance to catch Covid-19, not in the least. As for vaccine development, none of the front-running candidates for a Covid-19 vaccine had anything to do with gain-of-function research.”
These candidates either used existing technology, such as an inactivated vaccine, or built on research conducted on other viruses, he says.
The conflict among scientists regarding the work done on the world’s deadliest viruses in BSL-4 labs raises another question: who is in charge of monitoring what is going on?
According to Koblentz at George Mason University, government oversight is critical to BSL-4 lab security, but, he says, the people working in BSL labs are the linchpin, highlighting the “insider threat” – as seen in the US anthrax attacks – as the greatest security challenge.
“One thing that US labs have is a personnel reliability programme, which is designed to monitor researchers to ensure they are not suffering from mental distress, financial distress. If someone has been radicalised or blackmailed, then you need to know,” he says. This is “not just about bioterrorism but also about preventing the theft of proprietary information or protecting intellectual property because some of this research and the samples people work with can be very valuable”.

Koblentz says much of that oversight is up to the BSL-4 scientists themselves, and Kurth in Berlin says a network among BSL-4 researchers already exists. “The family of BSL-4 research is very small. We know each other, we meet regularly.”
Kurth says no BSL-4 lab in Europe has a staff of more than 50, in contrast to North America, he says. Smaller teams reduce risk of rogue personnel or sabotage, though “there is never 100 per cent certainty” when it comes to lab security.
But for practical global oversight and verification of BSL-4 labs, Attaran says, “There isn’t a good international inspection regime, which is terrifying.”
The International Atomic Energy Agency (IAEA) was set up to monitor and prevent the military use of nuclear technology and has 171 member states; the Organisation for the Prohibition of Chemical Weapons has 193 member countries working to eliminate chemical weapons, according to its mandate. But Attaran does not think the WHO is the right body to police global biosecurity: “I do not believe for a moment it is within WHO’s competence to do that.” However, he feels the first step should be a moratorium on gain-of-function research, and that would be best achieved through the WHO.
Franz, formerly of Fort Detrick, also does not see a biosecurity system under the WHO as the answer, because it is underfunded and understaffed. Koblentz says any organisation created to prevent proliferation of biological weapons would have special headaches.
“You can’t have a bio-IAEA because it would have to inspect tens of thousands of locations,” he says. “It would just not be feasible.”
Biodefence facilities
For Taiwan – which has two BSL-4s, as does mainland China – the facilities were essential when it came to dealing with the Covid-19 outbreak, says Ye Minggong, the former research director at the Ministry of National Defence’s BSL-4 lab.
“The labs are there to serve the country whenever it is facing an epidemic or needs to develop some special vaccine or test kits,” he says, attributing Taiwan’s investment in BSL-4 labs to its international isolation. “Taiwan is not a part of WHO, which means it cannot access a raft of information such as the origins of a virus.” This also means Taiwan cannot ask other countries to test deadly virus samples.
At the outset of the Covid-19 outbreak, Ye says, “Initially WHO said there was no human-to-human transmission, but then they realised this virus was highly infectious. If we had had no BSL-4 labs of our own at the time, our researchers could have easily been infected.”
The lethal nature of pathogens such as Ebola and their greater incidence in Africa led virologist Jean Bernard Lekana-Douki to call for more BSL-4 labs to be built on the continent. Ebola causes haemorrhagic fever and kills on average 50 per cent of those it infects, compared with fatality rates of less than 1 per cent for Covid-19.
“Because of global warming, climate change, lots of viruses and lots of pathogens will emerge; we need BSL-4 labs to give an adequate response,” says Lekana-Douki, director general of Gabon’s BSL-4 lab at the Centre Interdisciplinaire de Recherches Médicales de Franceville (CIRMF). But because of the controversy around gain-of-function research and accidents involving BSL-4 labs, not all researchers think the correct strategy is to build more, even faced with the threat from unknown viruses.
Richard Ebright, professor of chemistry and chemical biology at Rutgers University, in New Jersey, who signed the Cambridge Working Group statement, is a critic of the expansion of BSL-4 labs in the US. “The immense costs of constructing and operating the BSL-4 facilities has been a dead loss,” he says. “Many hundreds of millions of dollars that could have supported valuable research instead have been wasted on largely unused, largely empty ‘white elephants’.”
Ebright says the anthrax letters in the US – a week after the 9/11 attacks – sparked renewed interest in building more BSL-4 facilities for biodefence purposes, driven by the same kind of geopolitical competition that triggers war rather than a desire to serve genuine public health needs.
“The US BSL-4 expansion has triggered an international arms race in BSL-4 expansion, first [in] Europe, and now Asia, all mindlessly constructing BSL-4 facilities, without performing needs assessments, and without having a need for more BSL-4 capacity, just to keep pace with the US,” Ebright says.
Biosafety level 4 laboratories worldwide
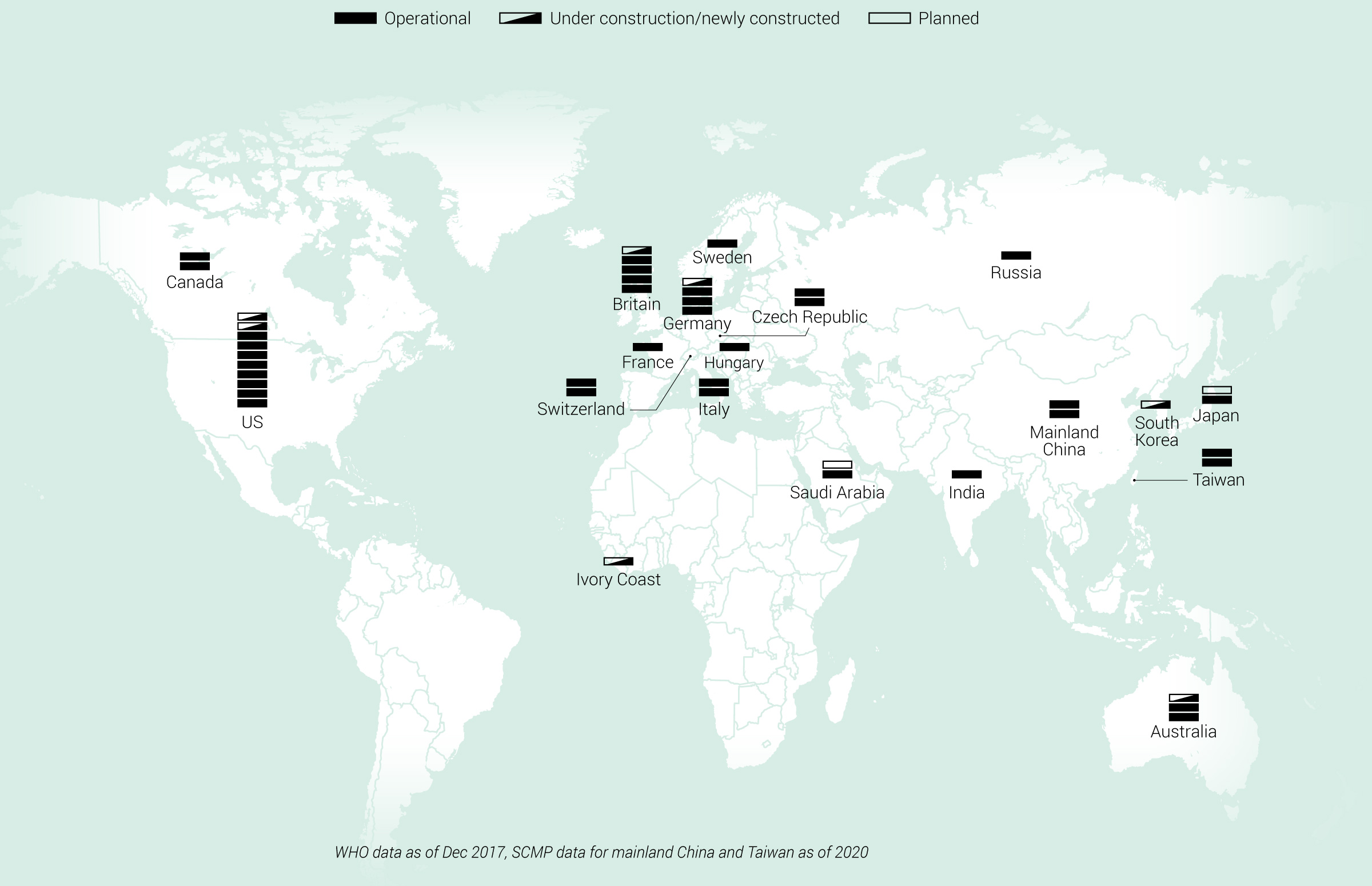
Juergen Richt, regents distinguished professor at Kansas State University’s College of Veterinary Medicine, says the labs are essential but also sees risk in their growing numbers. “If you have more people involved and you have more facilities then you have more human error.”
However, he says, the 9/11 attacks spurred the building of a bigger biodefence programme in the US because the threat was present and there was a need to work on potential antidotes and vaccines in BSL labs. “If you don’t have these facilities, you can’t do it,” he says.
The US anthrax attacks were a factor in Germany’s investment in BSL-4, too, according to Kurth, whose Berlin lab opened in 2018. And since the Sars outbreak in 2002, China has built two BSL-4 labs – one in Wuhan, another in Harbin. In 2016 the government announced plans to have as many as seven by 2025. But suspicions abound.
“The plan to build five or seven additional ones, when their original plan of three labs isn’t even done yet just raises the question of what these labs are going to be doing,” says Koblentz. “If the Chinese concern is being prepared for detecting a new outbreak, most of that can be done at the BSL-3 level and those would be public health labs that would be doing diagnostics and doing tests.”
The BSL-4 lab in the northeastern city of Harbin – where Unit 731 was headquartered – specialises in animals and livestock-related viruses, such as bird flu. The Wuhan Institute of Virology cost US$44 million and took about a decade to build, opening in 2018, according to the US State Department. It focuses on Sars and other viruses.

French scientists advised on the lab’s construction and the Wuhan staff were trained in France and the US. Its researchers include Shi Zhengli, a world renowned authority on viruses in bats, which are believed to have been the source of the Sars and Covid-19 pathogens.
For her work in the lab as well as years in the field trekking into isolated caves to collect samples, during which time she helped uncover the link between bats and Sars, she earned the moniker “bat woman”. However, her reputation was attacked when the Wuhan BSL-4 lab became a centre of controversy in the Covid-19 outbreak.
US officials, including Secretary of State Mike Pompeo, suggested the virus causing the pneumonia-like Covid-19 disease that first surfaced in Wuhan might have escaped from the BSL-4 lab. No evidence has been publicly produced to back up this allegation and Shi, as well as scientists in the US, Europe and elsewhere have dismissed it.
An analysis in the journal Nature noted the virus had none of the hallmarks of genetic engineering. The Wuhan Institute did identify the closest known relative to the Covid-19 pathogen, a bat virus that shares some 96 per cent genetic similarity. Scientists estimate the two viruses shared a common ancestor, but that would have been decades ago.
However, some of China’s own scientists have raised questions about safety at the facilities. The country lacks comprehensive legal and regulatory standards and is short of trained and experienced specialists, noted professor Wu Guizhen of the National Institute for Viral Disease Control and Prevention, in China’s Centre for Disease Control and Prevention, in a paper published last year.

The lack of specialised biosafety managers and engineers makes it difficult to identify and mitigate potential safety hazards, wrote Yuan Zhiming, a professor at the Wuhan Institute of Virology and the director of its BSL-4 lab, in another paper published in the same year.
Ye in Taiwan feels the deterioration in relations between China and the US will also throw up problems for the mainland’s BSL facilities. He doubts training opportunities in the US will remain open to Chinese scientists and believes BSL-4 labs will be hard-pressed without access to US technology.
“There are other places you can buy your equipment,” he says. “But the United States is the best, and it’s not good practice to mix equipment from different countries.”
Ebright at Rutgers University says that without an international means to enforce transparency, BSL-4 labs can become tools for authoritarian governments. “A crucial first step for China is to permit an open international investigation of the origins of Covid-19,” he says.
The Covid-19 pandemic is what the WHO warned was coming in its disease preparedness plan in 2018, when it listed the pathogens posing the greatest public health risk – including Disease X.
Former US Army medical researcher Franz says that during his career he attended many conferences on global threats to humanity and the nuclear risk took precedence, because the image of the mushroom cloud above Hiroshima had shown the world the catastrophic destructive power of an atomic bomb.
“The nuclear threat has long been seen, among security experts, as significantly greater than the threat of disease,” he says, “therefore leadership’s focus and preparation for a pandemic has received much less attention than nuclear policy.”
Covid-19, he says, could be the “mushroom cloud” that changes all that.
Source – south china morning post


Comment